Warning : Use the following information at your own risk. While accuracy is one my goals, there is always the possibility that some of the information could be wrong. There could be typos. I could also be severely mistaken in some of my knowledge. This site is meant to help clarify certain concepts of ECG and at no point should any life-or-death decision be made based upon the information contained within. Remember, this is just some page on the internet. (If you do find errors, please notify me by feedback.)
Junction here refers to the AV junction, the area around the AV node and the bundle of His. The exact definition of the AV junction often varies, depending on who you ask. As I've mentioned before, the AV node is an electrically conducting path that connects the atria to the ventricles. Emerging from the AV node is the bundle of His (also called the AV bundle). Because the "anatomy people" seem to disagree on where the AV node starts and stops, the "physiology people" call the general area the AV junction. This would include the AV node and at least part of the bundle of His.
|
|
|
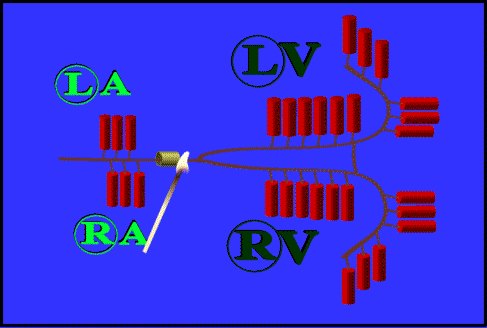
Figure 7-1 : A firecracker showing the firing of a junctional pacemaker |
What is a junctional rhythm? A junctional rhythm is one that starts in the AV junction.
Figure 7-1 illustrates what happens when a pacemaker in the junction fires. The match lights the fuse, causing the fire to travel both ways. In the atrial part of the fuse, the activation travels in the reverse direction (from right to left on the diagram). We know that when it travels "forward" it produces an upright P-wave. When it travels retrograde (which is a snooty, polysyllabic way of saying "backward"), the P wave is inverted (i.e. upside down, below the isoelectric line). Thus, an inverted P wave strongly indicates that the electrical impulse originated in the AV node or beyond.
In addition to being upside-down, the junctional P wave may not be before the QRS. When the sinus fires, the atria are depolarized before the ventricles, and thus the P wave is first. In figure 7-1, the atrial explosives are lit before those of the ventricles. While simply looking at the figure, however, it is hard to predict which set of explosives will be ignited first. Perhaps they will be ignited at the same time. The ignition of the explosives in the atria (i.e. atrial depolarization) is the P wave while the ignition of the ventricular explosives (i.e. ventricular depolarization) is the QRS complex. In a junctional rhythm, the P wave may occur before, during, or after the QRS complex. This depends on the exact location of the pacemaker, which may vary. When two waves occur at the same time, they add together. Anything above the isoelectric line counts as positive, below negative. Because the P wave in this case is negative, it will subtract from whatever the QRS is.
![]()
Premature Junctional Complex
A premature junctional complex (PJC) is not a rhythm but rather denotes a complex caused by a junctional pacemaker that interrupts the underlying rhythm.
|
|
|
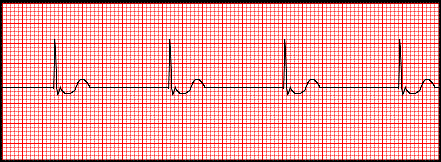
Figure 7-2 : Sinus rhythm with a PJC |
See Section 10 : Premature Complexes.
![]()
Junctional escape
We have talked about the "backup" pacemakers in the heart. There happens to be one of these pacemakers in the AV junction. This junctional pacemaker's intrinsic rate is between 40 and 60 times/min. Remember the rule, "the fastest pacemaker calls the shots"? That means that the sinus pacemaker (usually around 75/min) will normally prevent the junctional pacemaker from firing. What might happen if the sinus rate were to fall to, let's say, 30 times/minute? Well, the junctional pacemaker may start calling the shots. We call this type of "backup rhythm" an escape rhythm. Junctional escape will often have a rate between 40 and 60 beats/min.
|
|
|
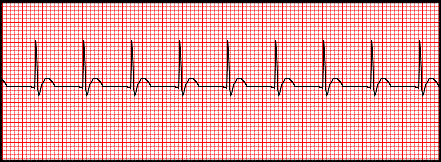
Figure 7-3 : Junctional escape |
![]()
Junctional tachycardia
(I am using the term junctional tachycardia to refer specifically to the type caused by a junctional pacemaker. The type of junctional tachycardias caused by reentry are dealt with in the PSVT section.)
Let's suppose an ectopic pacemaker in the AV junction decides to overtake the sinus node. This is equivalent of a coup, led by the a trouble maker in the AV junction. If the rate is faster than 100, we call this junctional tachycardia.
|
|
|
Figure 7-4 : Junctional tachycardia |
![]()
Accelerated junctional rhythm
Occasionally, an ectopic pacemaker in the AV junction will have a rate that is too fast to be considered junctional escape but too slow to be considered junctional tachycardia. We call this an accelerated junctional rhythm.
|
|
|
Figure 7-5 : Accelerated junctional rhythm |
©2004 Mauvila.com