Warning : Use the following information at your own risk. While accuracy is one my goals, there is always the possibility that some of the information could be wrong. There could be typos. I could also be severely mistaken in some of my knowledge. This site is meant to help clarify certain concepts of ECG and at no point should any life-or-death decision be made based upon the information contained within. Remember, this is just some page on the internet. (If you do find errors, please notify me by feedback.)
|
|
|
Figure 9-1 : A firecracker showing a number of potential ventricular pacemaker locations. Note that the fuse representing the ventricular septum is a "slow fuse". |
Several matches have been drawn in figure 9-1 to represent some of the possible locations of the ventricular pacemaker. These are all portions of the Purkinje system. Pick one of the matches and predict the path the impulse (fire) would follow. Perhaps can now imagine why impulses that originate in the ventricles produce wide QRS complexes. In a normal sinus beat, the impulse forks at the bundle of His. It covers both ventricles simultaneously. It generally depolarizes the ventricles in less than 0.10 seconds. If you imagine that the impulse starts where the bottom match is lighting the fuse, you can see it now has to cover both ventricles. The "slow fuse" is where the impulse can travel through the ventricular septum and into the other ventricle. This should explain why ventricular pacemakers cause a QRS complex longer than 0.10 s.
What else might cause a QRS to last longer than 0.10 seconds? Imagine that one of the bundle branches were blocked. (The bundle branches start at the fork, just after the A.V. node.) An impulse that originates in the sinus node would be normal up until it reaches the block. If the impulse could only travel down ONE of the branches, it would have to cut over through the ventricular septum ("slow fuse") to depolarize the other ventricle. You can see why this would take longer. Not everything that glitters is gold, and not every QRS that is wide is caused by a ventricular pacemaker.
All QRS complexes of ventricular origin are wide (> 0.12 s). Does it logically follow that all wide QRS complexes are ventricular? No, it does not. In fact, it is the case that NOT ALL WIDE QRS COMPLEXES ARE FROM THE VENTRICLES. On the other hand, virtually all narrow complex QRS complex are supraventricular (i.e. not from the ventricles). If this didn't "click," you might want to reread this paragraph.
Let's say we can put all rhythms in one of two categories : supraventricular or ventricular.
Supraventricular QRS complexes : NARROW or WIDE
Ventricular QRS complexes : WIDE only
![]()
Premature Ventricle Complex
Premature ventricular complex (PVC) is a term that originally was called premature ventricular contraction. Because the mechanical contraction of the ventricles cannot be inferred from the ECG, the word complex has replaced contraction.
These are also referred to as : premature ventricular beats (PVB), VPBs, and VPCs.
PVCs tend to be compensating (i.e. they don't travel back and reset the underlying pacemaker). In these cases, the distance from the normal P wave before the PVC to the P wave after the PVC is twice the underlying P-P interval.
Unlike the other three rhythms in this section, PVCs frequently occur in normal healthy hearts and often go unnoticed. They also may give a person the feeling of having "skipped a beat". On the other hand, PVCs in an unhealthy heart may be a bad omen.
|
|
|
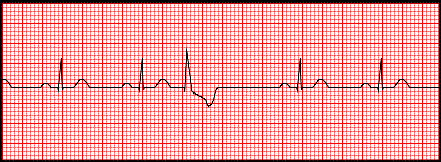
Figure 9-2 : Sinus rhythm with a unifocal PVC |
PVCs are also covered in Section 10 : Premature Complexes.
![]()
Ventricular fibrillation
Ventricular fibrillation ("v-fib", often abbreviated VF) describes the electrical activity associated with the quivering of the ventricles. When Don Corleone is shot, quivering Fredo is unable to successfully wield a gun. Quivering ventricles are about as effective as quivering Fredo- they cannot pump blood. I mentioned earlier that, while functional atria are a prerequisite for playing tennis or jogging, functional ventricles are a prerequisite for staying alive. Thus, untreated v-fib can progress to death within minutes. You can understand why v-fib is one of the evil rhythms. When someone suddenly drops dead from a cardiac arrest, v-fib is likely to blame.
The pattern for ventricular fibrillation is... well, there really is no pattern. It is random electrical activity. Sometimes the amplitude of the waves is large (coarse VF), while other times the amplitude is so small (fine VF) that the rhythm is almost asystole. It has almost a "kindergarten artwork" quality to it.
As the minutes pass, cells in the body become damaged due to the lack of oxygenated blood. Among these are cells of the heart. As the heart dies, it loses its ability to conduct electricity. Coarse v-fib will turn into fine v-fib, and fine v-fib will transition into asystole.
|
|
|
Figure 9-3 : Ventricular fibrillation (coarse) |
|
|
|
Figure 9-4 : Ventricular fibrillation (fine) |
![]()
Ventricular tachycardia
Ventricular tachycardia (V-tach, often abbreviated VT) refers to a rhythm that arises from the ventricles causing the heart to beat at a rate faster than 100 beats per minute. The ventricular rate is usually above 120 beats/min and may exceed 250 beats/min. At some point, the ventricles may beat so frequently that there is not adequate time for the blood to refill. A patient in ventricular tachycardia MAY or MAY NOT have a pulse.
A heart in VT is vulnerable to going into ventricular fibrillation. In fact, the common sequence of arrhythmias in patients who die in this rhythm is: V-tach to V-fib to asystole.
The QRS complex will be wider than 0.12 seconds. Figure 9-5 shows the stereotypical V-tach, but not all cases look like this.
Unless you have been trained to distinguish a ventricular QRS complex from a wide QRS of non-ventricular origin, then you should call a tachycardia with wide QRS complexes a "wide complex tachycardia."
|
|
|
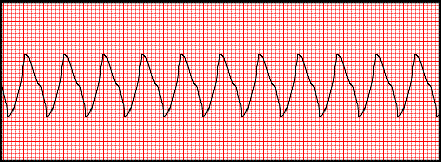
Figure 9-5 : Ventricular tachycardia |
![]()
Ventricular escape
Ventricular escape, often called idioventricular escape, is when an ectopic "backup" pacemaker in the ventricles kicks in. A few things can cause this :
- The sinus and junctional pacemakers have failed
- There is a block that prevents impulses of the sinus (or junctional) pacemaker from reaching the ventricles.
Although it is considered a "backup" rhythm, it is only slightly more compatible with life than asystole. The intrinsic rate of a ventricular pacemaker is 20 - 40 times/minute. In other words, this is a very bad rhythm.
|
|
|
Figure 9-6 : Idioventricular rhythm |
![]()
Asystole
Asystole is not a ventricular rhythm. It is the "flat-line"; subsequently, it is the easiest rhythm to recognize. Because it has no electrical activity, asystole does not readily belong into any of the other groups of arrhythmias. I have included in this section because it is often the end result of ventricular fibrillation.
Pronounced uh-SIS-toe-lee.
Always make sure the equipment is connected to the patient. Also, check more than one lead to confirm that the rhythm is asystole. If an electrically active heart has all of its activity perpendicular to a given lead, very little will show on that lead's ECG. In these cases, another lead (pointing a different direction) should pick up on this hidden activity.
|
|
|
Figure 9-7 : Asystole |
©2004 Mauvila.com